The U.S. is returning to the fold of global health cooperation. President Joe Biden’s administration has reversed a decision to leave the World Health Organization and signed up to COVAX, a 92-nation vaccine collaboration snubbed by his predecessor. It’s a major boost for the global rollout of multiple safe and effective vaccines, seen as the best shot at an endgame to the COVID-19 pandemic.
Getting there will require altruism at a time of great pressure to act selfishly. Doses are a scarce, finite resource right now. Rich countries with deep pockets have the advantage in buying and deploying them, especially given the complexity of vaccine logistics. It wasn’t so long ago that countries were desperately outbidding their allies to secure masks and medical equipment. Programs like COVAX, which has secured almost 2 billion doses to vaccinate up to a fifth of countries’ populations by the end of 2021, are going to be vital.
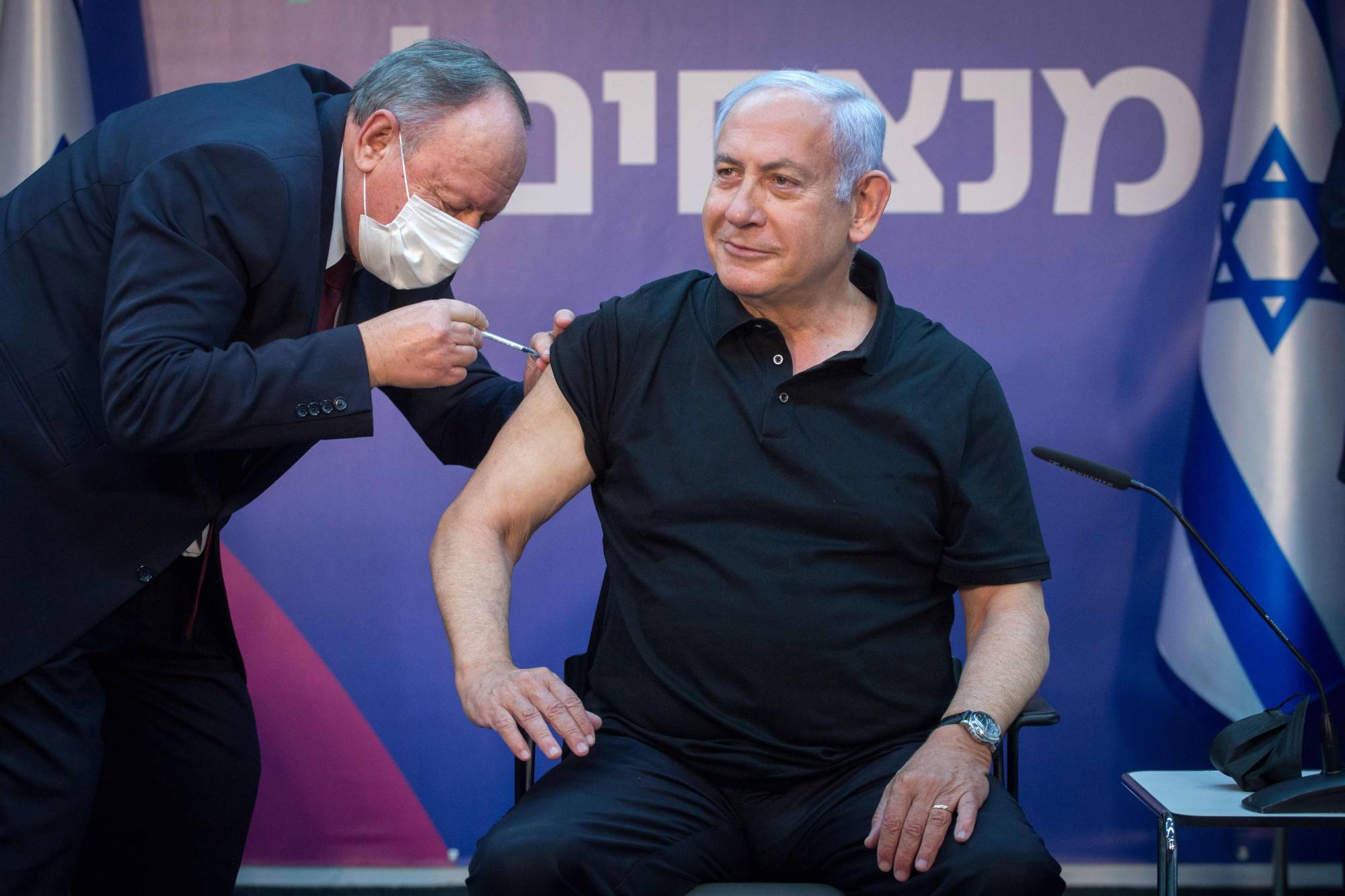
Money for doses isn’t the only key, though. In the 21st-century vaccine economy, data is also power. Tiny Israel is set to immunize its population months before far bigger and richer countries, partly by ordering early — and reportedly at a higher price — but also by sharing patient information after vaccination. Deliveries of Pfizer Inc. and BioNTech SE’s COVID-19 vaccine were expedited earlier this month after a deal to share extensive data on the inoculation program, according to colleagues at Bloomberg News.

















With your current subscription plan you can comment on stories. However, before writing your first comment, please create a display name in the Profile section of your subscriber account page.