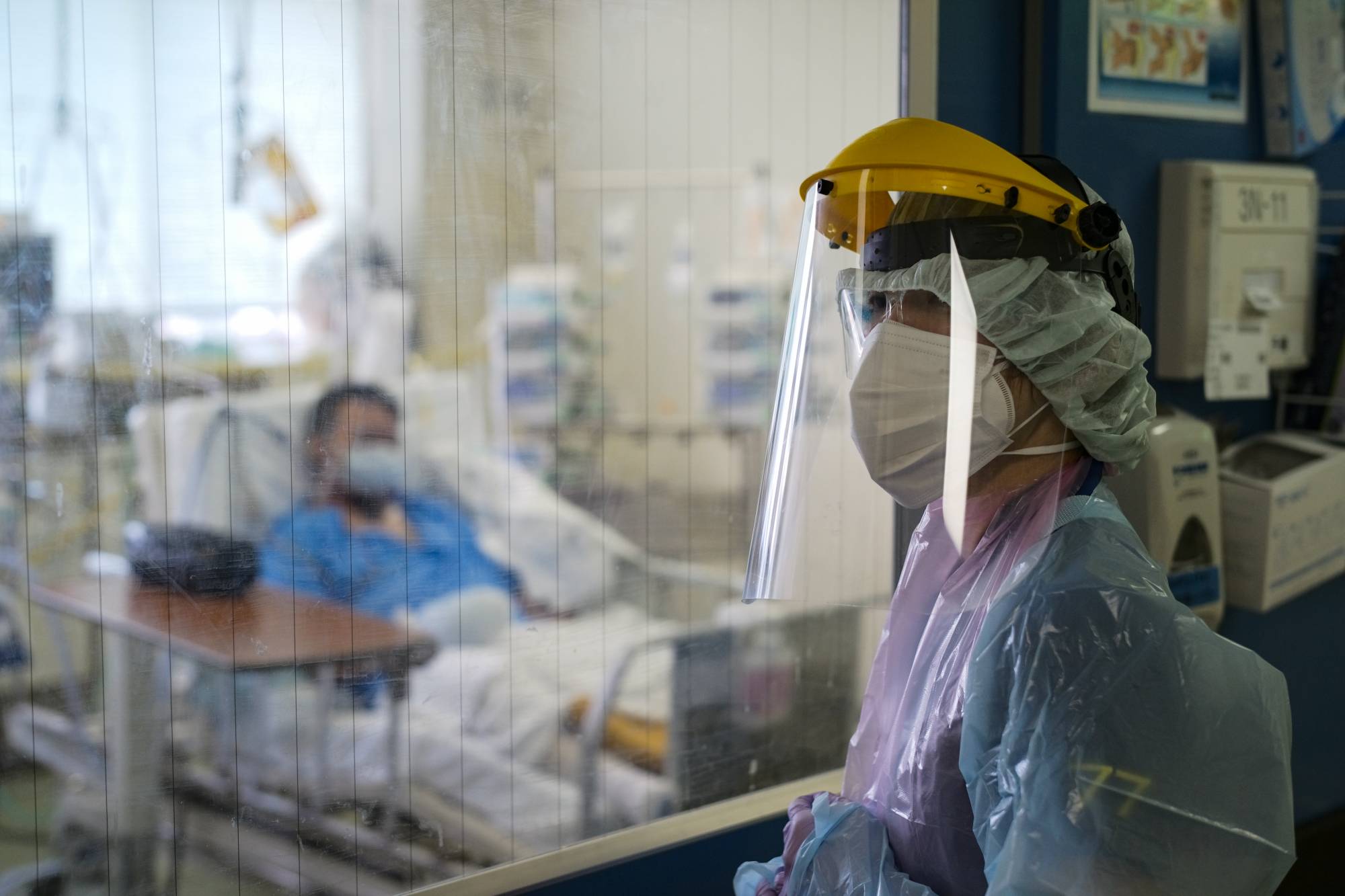
Donning the protective gear required to enter the pressurized hospital room of a COVID-19 patient has become second nature for Nao Watarumi.
The 38-year-old nurse was performing a routine check on a patient, a man in his 50s who had been receiving artificial ventilation for close to a week in the coronavirus ward of Itabashi Hospital in Tokyo.
“It used to take us a long time to gear up every time we needed to go in and out of a room to check on a patient, but now we can usually do it in less than five minutes,” she said after she emerged from the patient’s room and began to methodically remove her goggles, gown, face shield and a second layer of gloves.


















With your current subscription plan you can comment on stories. However, before writing your first comment, please create a display name in the Profile section of your subscriber account page.