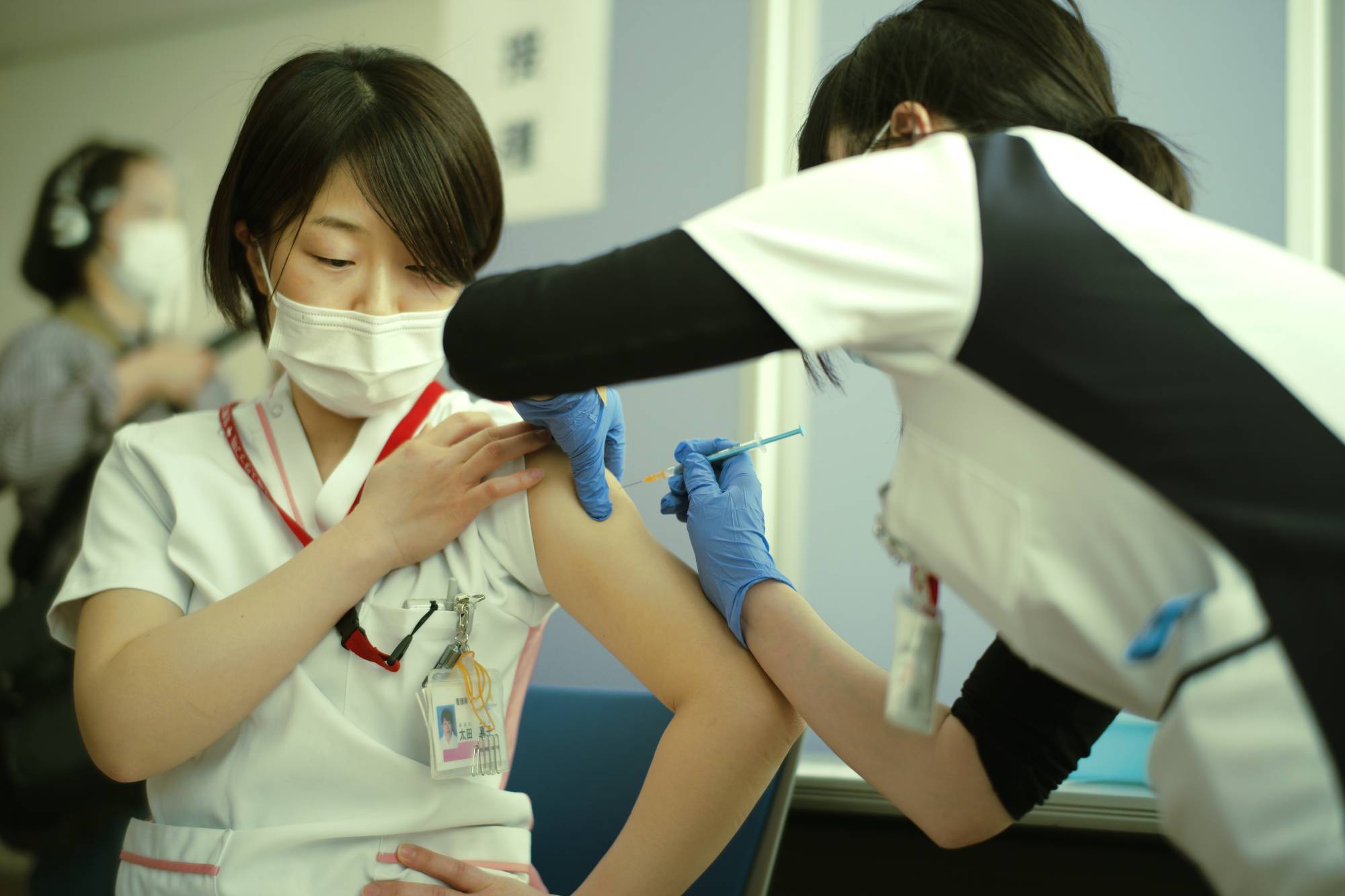
Japan’s slow coronavirus vaccine rollout has again shed light on the cautious process in place for vaccine approval in the country, reigniting the question of how to balance drug safety with the need to combat a public health crisis in a speedy manner.
This challenge seemed to be on the mind of Prime Minister Yoshihide Suga when he acknowledged criticism of the nation's inoculation program during a news conference last month.
“Most countries overseas don’t need to conduct domestic clinical trials for vaccines, but Japan does,” Suga told reporters. “I strongly feel that we need to revise laws to better respond to this kind of emergency situation.”