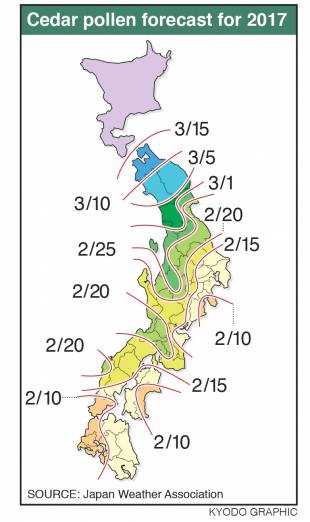
About a quarter of the population is bracing for an attack from a seemingly innocuous source — pollen.
The perennial release of cedar pollen, which hits much of the archipelago between February and May each year, triggers an allergic reaction in about 1 in 4 of Japan’s population of about 126 million people. Fits of sneezing abound as noses either clog or run freely, and eyes become so itchy there's a temptation to scratch them from their sockets.