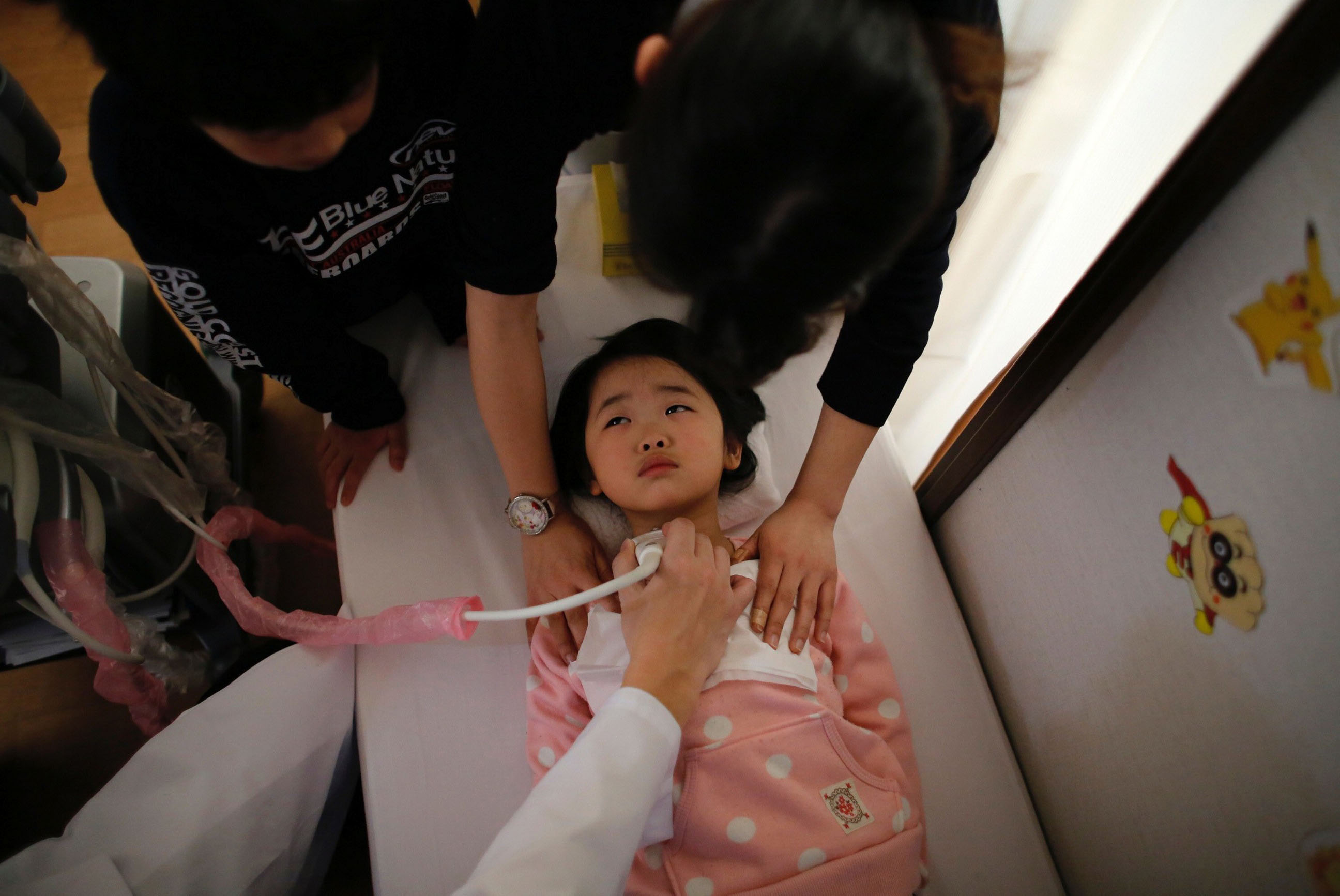
More than three years after the triple core meltdown in Fukushima Prefecture devastated the lives of thousands of residents, the effect that the radiation release is having on children's thyroid glands still weighs heavily on residents' minds.
The iodine-131 released into the air by the meltdowns accumulates in the thyroid gland, increasing the risk of thyroid cancer. The gland is responsible for regulating hormone levels in the body.
Children are considered especially vulnerable. After the 1986 Chernobyl disaster, more than 6,000 children were diagnosed with thyroid cancer by 2005, according to the U.N. Scientific Committee of the Effects of Atomic Radiation.